Healthcare Contract Management
Audit payer compliance against contract terms and boost revenue
Unfortunately, missed payer payments and underpayments happen. Identifying and correcting these inaccurate payments often falls to healthcare providers. These errors can cause stress and volatility to your revenue cycle.
Simple human error is the main reason why medical claims are denied. The smallest typo or discrepancy can lead to an immediate denial, and reworking a claim rarely increases its chance of being more accurate. Streamline claims management by checking that every claim is clean and error-free before it is submitted. Fewer denials and reworked claims mean a faster and more predictable revenue cycle, as well as lower administrative costs and more time for staff to focus on patient care.
You need automated access to the right data. Our healthcare contract management solutions help you get reimbursed accurately and quickly, while strengthening your relationships with payers.
Timothy Daye, Director, Managed Care Contracting at Duke Health Integrated Practice, shares how Experian Health's Contract Manager solution helps their organization protect revenue.
Audit payer contract performance to assure compliance - and maximize revenue.
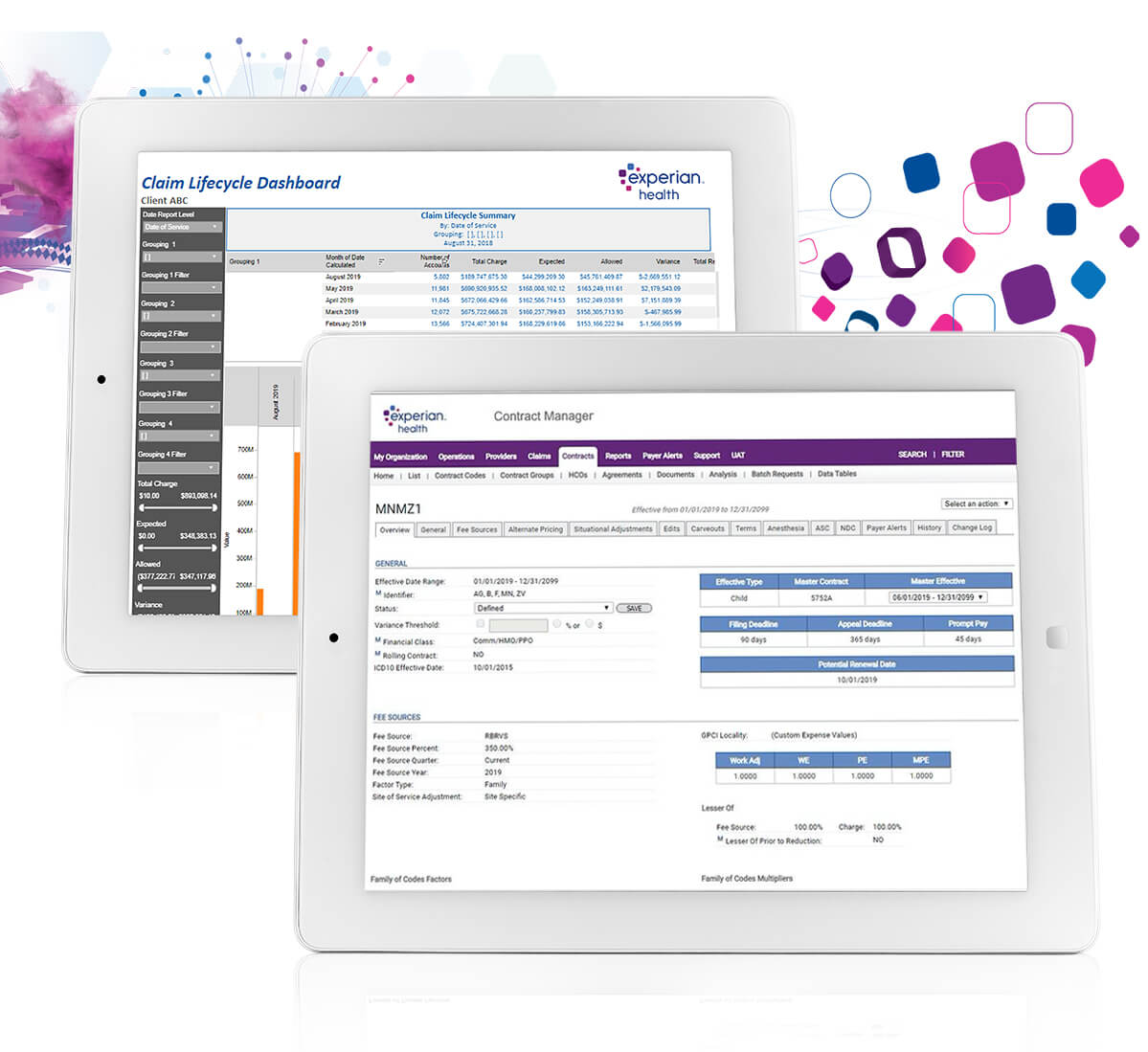
Our healthcare contract management solution seamlessly integrates with many hospital information systems. By automatically populating accurate rates and authorization rules, you minimize errors and maximize efficiency, reducing the need for manual data entry and rework.
Imagine never missing out on reimbursements due to buried contract clauses or errors. Payer contract management empowers you with automated oversight of your payer contracts. It validates reimbursement accuracy by comparing expected allowed amounts to actual allowed amounts. Contract Manager quickly and efficiently pinpoints variances to ensure your organization is paid per contract terms and payment policies., helping you maximize revenue recovery. This translates to improved cash flow and reduced administrative burdens. It also allows your staff to focus on patient care.
Whether you're a small clinic or a large hospital network, healthcare contract management can simplify any complex contract and streamline workflows. Its user-friendly interface and configurable dashboards make it easy for staff of all technical backgrounds to access and utilize the system effectively. Contract Manager enables users to audit claims across an entire organization – whether one medical group or a large health system – in a single solution to improve overall payer contract management efficiency
Staying compliant with ever-evolving healthcare regulations can be a challenge. Contract management software for healthcare helps you stay ahead of the curve. Our built-in features and automated alerts ensure your contracts adhere to the latest regulations. Proprietary valuation logic including client-specific claim to contract mapping logic that utilizes a broad number of claim elements for more precise valuation. This proactive approach reduces the risk of audits and penalties, giving you peace of mind.
Stop leaving money on the table due to missed reimbursements or underpayments. Payer contract management identifies discrepancies between the amounts you bill, and the rates agreed upon in your payer contracts. This automation minimizes revenue leakage by highlighting potential errors and ensuring you receive the full and accurate reimbursement you deserve.

Experian Health’s Contract Manager and Contract Analysis product has been ranked #1 in the 2026 Best in KLAS: Software & Services report, for the fourth consecutive year.

What happens when payers don’t comply with contract terms? What if a provider overlooks the fine print? Contracts between healthcare providers and payers are supposed to make each party’s responsibilities crystal clear.

Providers are grappling with mounting complexity, an explosion of data, and continuing pressure to maximize efficiency and revenue.

Effective contract management for healthcare organizations is pivotal in this complex and highly regulated world. Healthcare organizations, whether large hospitals, clinics, or individual practitioners, contract with various entities, including vendors, insurance providers, and regulatory bodies.