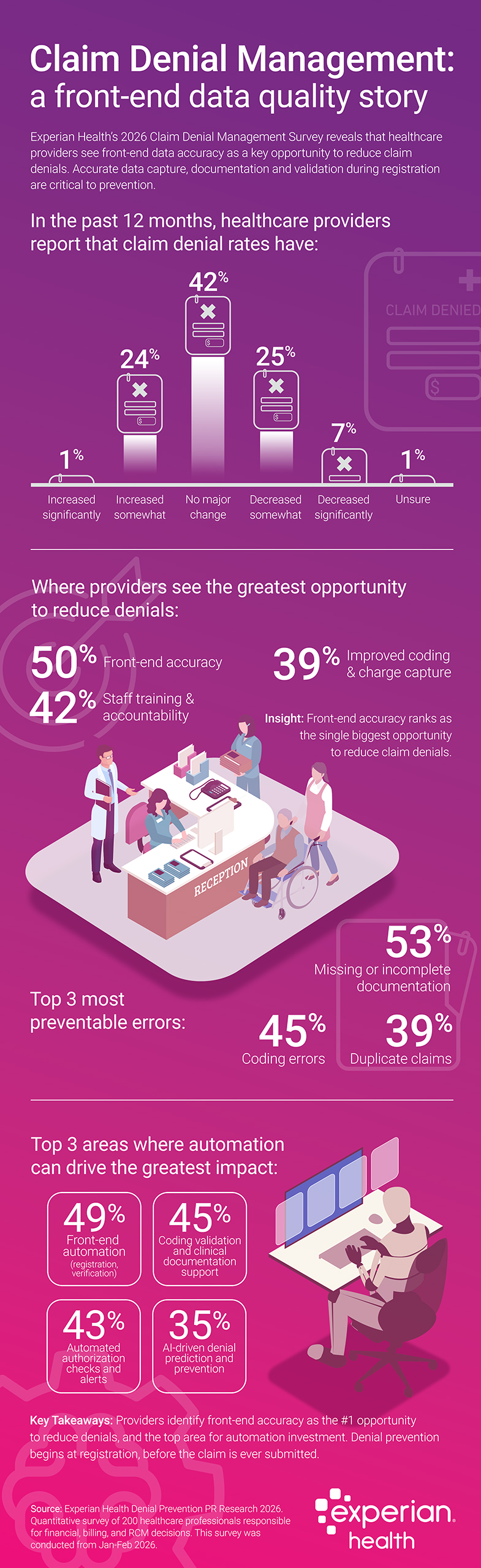
Claim denial rates remain high – and in some cases, they’re rising. Experian Health’s latest Denial Management survey found that over the past 12 months, 25% of healthcare providers reported increased denial rates, while 42% saw no meaningful change.
At the same time, there’s an opportunity for improvement. 50% of healthcare organizations identify front-end accuracy as a key opportunity to reduce denials. Incomplete documentation, coding, and eligibility errors rank among the top 5 most preventable causes of claim denials. The implication is clear — many denials stem from preventable data gaps that are introduced before a claim is ever submitted.
The research shows that denial prevention and stronger claims management begin at the front end. When asked where automation would have the greatest impact, respondents pointed to front-end and coding validation, automated authorization checks, and AI-driven denial prediction and prevention.
Denial management is fundamentally a front-end data integrity strategy. Preventing and reducing denials begins at registration. Healthcare organizations that shift from denial response to denial prevention – prioritizing accurate and complete front-end data capture – will see more sustainable reductions in denials, improve revenue predictability and ease administrative burdens across the revenue cycle.